This post was originally published in Birthspirit Midwifery Journal 2009; 1: 43-46. Updated February, 2014
Each of Jaynie’s three labours built up over several days before she had contractions that were frequent enough for her to determine she was in labour. During these times she carried on with everyday activities such as attending yoga classes in her first labour and home-schooling her two daughters during the third. This period of labour was valued and enjoyable for Jaynie, spent predominantly in intimacy and seclusion with her family.
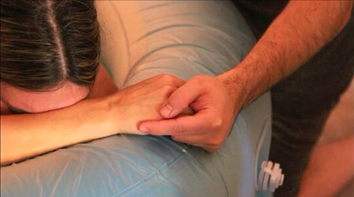
Jaynie liked midwife attendance in labour when contractions were intense but the midwife belonged on the periphery of the birth space. Jaynie’s husband, Ken, provided all the physical and emotional support with the midwife there to provide only the patient vigil. Jaynie had a deep connection with her babies throughout the continuum of childbearing so gaining affirmation of the baby’s wellbeing was through her comments about the baby’s movements and hiccups with minimal aid of a Pinard stethoscope.
youtube.com/watch?v=HFzam3HFjnE
If one were waiting for the anxiety of transition that is predicated in many texts, the midwife would miss the forerunner to Jaynie pushing as the spacing out of contractions is the only sign that birth is near. It is when Jaynie begins to shorten her quiet outward breath with almost imperceptible pushing that the baby’s imminent birth is signalled. With her first two births the urge to push “came out of nowhere”; during the third, she was conscious of pushing because she was tired and wanted the labour to end. Jaynie’s waters normally go within the last few moments of labour and the heavy show, often attributed to full dilation, appears moments before the baby’s head. As a sufferer of endometriosis prior to having children, Jaynie’s ability to deal with pain had already been fully tested prior to her first baby.
When her second and third babies were born she lifted one to the surface of the water herself and drew the other close after being handed to her. Her babies are ‘in arms’ babies. They sleep and rest in her arms, cheek on bare breast or in the arms of another family member.
The benefit of hindsight of having attended two of Jaynie’s three home births, and hearing the story of her first birth along with reading the midwifery notes of that birth, allows me to see the pattern over these three births. However, listening to Jaynie tell the story of her first labour and birth was disturbing for me the first time I cared for Jaynie in her second pregnancy. Evident in her story was a cascade of intervention – not the usual induction or augmentation of labour with vaginal prostaglandins, Syntocinon infusion, epidural anaesthesia and operative or surgical birth. This was a home birth story that Jaynie related, complete with of a cascade of intervention, as follows.
For this first baby, Jaynie’s labour rhythm developed over two days. She arranged in the evening of the second night for the birth pool to be dropped off before bathing and going to bed. She couldn’t sleep after 4am and used the pool for relaxation and pleasure – a pleasure still evident in her smile at this point as she related her birth story to me. Soon after the midwife’s visit at 9am Jaynie was examined vaginally and her cervix was estimated to be 6-7 centimetres dilated.
Jaynie felt pressure from the midwife to progress in labour and took the cell salts Mag Phos and Calc Phos which were recommended to strengthen and speed contractions. These made Jaynie’s contractions more intense. When the vaginal examination was repeated four and a half hours later, her cervix had opened to be 7-8 centimetres and the baby had moved down to be at Station 0. This was seen by the midwife as not enough progress and Jaynie’s waters were artificially ruptured following which she was given the homeopathic Lobelia 200c to assist retraction of a thin lip of cervix.
Jaynie used the pool after this time and, while the midwife noted labour slowed, Jaynie felt it was strong in the pool. With all the focus on making labour stronger by artificial rupture of membranes (ARM), cell salts, homeopathy and different positional techniques, the toilet was the only place she and Ken felt they could be alone, and Jaynie intermittently sought sanctuary there.
She was examined vaginally for a third time in seven hours as she wanted to push. This was a phase that Jaynie remembers as wanting to lie down and relax but she was urged by the midwife to be upright as the latter had a sense of urgency that the baby had to be born, the reason for which was not reflected in the midwifery notes. It may well have been the presence of meconium which became known with membrane rupture as abnormal heart tones were not indicated in the midwifery notes. The midwife’s concern was enough for her to get Jaynie to leave the birth pool where she had been relaxing, and onto a floor mattress. Jaynie pushed expulsively on the thin anterior lip of cervix and her first daughter was born in three pushes while the midwife performed perineal massage.
There was a brisk 500 ml blood loss estimated. Jaynie had wanted the umbilical cord to remain attached to her daughter’s placenta but now the midwife’s focus turned to the birth of the placenta. The umbilical cord was clamped and cut, and an intramuscular injection of Syntocinon was administered without Jaynie’s permission.

http://www.flickr.com/photos/timtom/1417336029
Her baby had immediately latched on, and was feeding determinedly. Jaynie felt very “scattered” with the multiple interferences of late labour and, while her baby still wanted to feed, she was instructed to give the baby to Ken so she could “be in her body to push”. This was to oblige the midwife’s need for placental birth to be achieved.
The blood loss had stopped as quickly as it had started and Jaynie’s uterus remained well contracted with minimal further blood loss. While there was no perineal trauma, bilateral labial tears were later stitched.
Jaynie was given Kali Carb 200c to prompt birth of the placenta.
After two unsuccessful attempts at controlled cord traction and with a Syntocinon infusion running, Jaynie was transferred to hospital two hours after the birth for manual removal of the placenta under epidural anaesthesia – a matter Jaynie felt she had no other choice than to make. Once manual removal was achieved, and with antibiotics administered, Jaynie was left to recover from this process which she described as “frightening and painful and leaving [her] feeling as if [she] had been invaded”.
While she was now finally able to focus on her daughter, the intimate family time that she and Ken had planned had to be abandoned as Ken was prevented by hospital staff from staying the night. He would spend the night in their van in the hospital car park.
Jaynie had wanted to be discharged immediately but felt exhausted and weak following the epidural and a shower, so stayed the night. She did not sleep at all overnight and spend these hours gazing at her treasured daughter. When she returned home at 7am, she, Ken and the baby went to bed for a week and were well supported by others who brought them meals.
Following the birth of her third and last child, I revisited all the midwifery notes and Jaynie’s first birth story. The discomfort I felt when she originally told me this first birth story percolated up again. The way she had laboured with her first baby and the time it took for her to do so were well within the bounds of my experience of a ‘normal’ labour. A smooth and progressive pattern of labour had been evident with the increasing strength and frequency of Jaynie’s contractions, her knowledge of the intensifying labour over the preceding time, and her hormonal state which necessitated her withdrawal from outside stimulus. This knowing of progressive labour would have been supported by ongoing descent of the baby’s head assessable through abdominal palpation and observation of her back, the lengthening and deepening burgundy of the buttock crease, and her increasing birth energy. After having attended many similar first labours, I could see no role for stimulation of such a labour with cell salts or homeopathic remedies.
It was (and is) equally difficult to see the need for artificial rupture of membranes based on vaginal examinations – a test known to be subjective, imprecise and poorly reproducible Downe et al (2013); Buchmann & Libhaber (2008) & (2007); Letic (2003). These examinations gave poor information. For example, Jaynie’s cervix was noted to have dilated to 6–7 cm with the first assessment and 7–8 cm with the second examination four and a half hours later. This one centimetre difference in each individual finding represented 16.6 percent and 14.2 percent variance, respectively. Further, the potential two centimetres increase in dilatation in four and a half hours – that is, up to a 33.3 percent increase – must be seen as ‘adequate’ as it spans the stage when, prior to seven centimetres dilatation, it is not uncommon for the cervix to remain unchanged for more than two hours in a first labour Zhang et al (2002).
Acting on the (mis)information found at vaginal examination initiated the cascade of intervention. It began with the use of cell salts and homeopathic remedies and was furthered with ARM – a surgical technique which has no place in a physiological labour Smythe et al (2013). Such interventions irrevocably alter labour and, for Jaynie, contributed to scattering the deeply internal hormonal and emotional connections within her labour. Consequences of these interferences were played out in the retention of her placenta which was firmly adherent in the fundus.
Had Jaynie been supported in a non-interventionist way in this normal labour, it is very probable that she would have given birth to her placenta within an hour as she did with the two births that followed. Jaynie would then have been able to flow the mamatoto (motherchild) of pregnancy, without disruption, into the attached parenting that underpins her mothering. And, finally, Jaynie’s plan for natural childbirth, devoid of unnecessary intervention, implicit in the decision to birth at home, would have been honoured.
